Even though the German shepherd likely had cancer, his health records show how little we know about animals and the coronavirus.

www.nationalgeographic.com
(fair use applies)
Exclusive: Buddy, first dog to test positive for COVID-19 in the U.S., has died
Even though the German shepherd likely had cancer, his health records show how little we know about animals and the coronavirus.
By Natasha Daly
PUBLISHED July 29, 2020
Buddy liked dog stuff: running through the sprinklers, going on long car rides, swimming in the lake. He cuddled the Mahoneys—his owners and family—at the end of tough days. He humored them when they dressed him up as a bunny for Halloween. He was a protective big brother to 10-month-old Duke, the family’s other German shepherd. He loved everyone. He lived up to his name.
In mid-April, right before his seventh birthday, Buddy began struggling to breathe.
Six weeks later, he became the first dog in the United States to be confirmed positive for SARS-CoV-2, the coronavirus that causes COVID-19. On July 11, Buddy died.
Medical records provided by the Mahoneys and reviewed for National Geographic by two veterinarians who were not involved in his treatment indicate that Buddy likely had lymphoma, a type of cancer, which would explain the symptoms he suffered just before his death. The Mahoneys didn’t learn that lymphoma was being considered as the probable cause of his symptoms until the day of his death, they say, when additional bloodwork results confirmed it. It’s unclear whether cancer made him more susceptible to contracting the coronavirus, or if the virus made him ill, or if it was just a case of coincidental timing. Buddy’s family, like thousands of families grappling with the effects of the coronavirus around the world, is left with many questions and few answers.
Until now, Buddy’s identity, the details of his case, and his death were not public. A press release issued by the U.S. Department of Agriculture (USDA) in early June revealed his general location (Staten Island, New York), his breed (German shepherd), his likely source of transmission (a COVID-positive owner), and his status (expected to recover). Public records for the few other pets to have tested positive in the U.S. are similarly sparse.
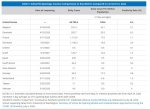
Upon announcement, Buddy’s milestone case appeared fairly open and shut, but the Mahoneys’ experience over the two and a half months between their dog’s first wheeze and his death was one of confusion and heartbreak. Their story puts a spotlight on the rare experience of being an owner of COVID-positive pet—a distinction shared by only a handful of individuals around the world. While more than four million people have been diagnosed with COVID-19 in the U.S., fewer than 25 pets have. There’s no rubric for how to navigate COVID-19 in your pet dog.
“You tell people that your dog was positive, and they look at you [as if you have] ten heads,” Allison Mahoney says. “[Buddy] was the love of our lives….He brought joy to everybody. I can’t wrap my head around it.” The Mahoneys say they are frustrated that health experts didn’t more closely probe possible connections between COVID and the cascading health problems. After Buddy’s diagnosis, Allison’s husband, Robert, asked New York City veterinary health officials, who were in charge of the case, whether they were interested in doing more testing on Buddy. Robert Mahoney says the officials never asked for further testing or exams.
The New York City Department of Health told National Geographic that because Buddy was severely anemic, it did not want to collect additional blood out of concern for the dog’s health, and that confirmation results indicate it was unlikely that he was still shedding virus—meaning he was probably no longer contagious—by May 20, when he was tested the second time. Buddy wasn’t tested after that date.
For humans, the signs and symptoms of infection vary widely. In some, its presence is barely a flicker. In others, it causes total organ failure. For many, it’s somewhere in between. Having an underlying medical condition increases susceptibility, doctors think. We’re learning more every day.
The narrative for the coronavirus in animals, however, has so far been consistent and narrow: They are rarely affected. When they do get the virus, it’s almost always from an owner. They have mild symptoms. They usually recover.
In reality, little is known about how the virus affects the typical pet dog.
The Mahoneys’ detailed accounts and Buddy’s veterinary records now comprise some of the most comprehensive and granular information the public has on an infected animal. Their story also sheds light on the gaps in public knowledge regarding animals and the novel coronavirus, highlighting what may be a need for a more unified, consistent approach to monitoring and investigating positive cases, and bringing that information back to the research community.
Buddy’s decline
When Buddy, who’d never been sick, developed thick mucus in his nose and started breathing heavily in April, no one except Robert Mahoney believed the dog might have COVID-19. Mahoney himself had been suffering through the virus for three weeks—he was weak, had a scratchy throat, and had lost his sense of taste. “They called me on Easter and said, ‘By the way, here’s your Easter gift: you’re positive,’ ” he recalls.
“Without a shadow of a doubt, I thought [Buddy] was positive” too, he says.
At first, it was difficult to find someone to examine Buddy. His usual vet wasn’t seeing patients because of the pandemic. Another local clinic wouldn’t allow Robert Mahoney to come into the office because he had COVID-19, so they prescribed Buddy antibiotics over the phone. Mahoney says the vet was skeptical that Buddy might have the coronavirus, and the office didn’t have test kits anyway.
The next week, Buddy was still struggling to breathe and had lost his appetite, so the Mahoneys’ 13-year-old daughter, Julianna, who had tested negative, was permitted to bring the dog into the office.
From April 21 to May 15, Buddy continued to lose weight. He became increasingly lethargic. The Mahoneys took him to three different veterinarians on Staten Island, none of whom thought the coronavirus was likely. He got an ultrasound and X-rays, which indicated an enlarged spleen and liver, and he saw a cardiologist, who detected a heart murmur. Buddy spent two and a half weeks on antibiotics and two heart medications, and he was subsequently put on steroids. At this point, Robert Mahoney says, Buddy’s doctors were still doubtful he had the coronavirus, and they had not yet identified lymphoma as a probable cause of his illness.
It was at the third veterinary clinic, Bay Street Animal Hospital, where Mahoney was finally able to have Buddy tested for COVID-19. That was on May 15, one month after Buddy’s breathing trouble began.
A few days later, the clinic called. Buddy’s test results were in: He was positive. Mahoney was told to bring both the family’s dogs to the clinic immediately because health officials needed to confirm Buddy’s results and test Duke, their puppy. When Mahoney arrived at the clinic with the dogs on May 20, he says that “they came greeting me looking like space martians with hazmat suits.”
“For us it was a shock factor for a moment there...how do we protect our staff?” says Robert Cohen, veterinarian at Bay Street who treated Buddy, because little is known about infected dogs’ ability to transfer the virus to other dogs or humans. “We were well-PPE’d,” he says, referring to personal protective equipment such as masks and gloves.
Officials collected samples from Buddy and Duke, then sent them home.
First dog to test positive
On June 2, the New York City Department of Health called Mahoney to tell him that Buddy had indeed contracted the virus. They confirmed that Buddy’s original samples collected on May 15 by his vet were positive for SARS-CoV-2, but the additional samples they collected on May 20 were negative, indicating that the virus was no longer present in the dog’s body, a department spokesperson told National Geographic. Duke had tested negative, but he did have antibodies, indicating he had been infected at some point.
Yet Buddy’s health continued to decline. He soon started urinating uncontrollably and had blood in his urine. Later that month, his breathing became so labored that it sounded “like a freight train,” Allison Mahoney says. In early July, Buddy began to have trouble walking.
Robert Mahoney took him back to the vet each time his health seemed to get worse, which was about every two weeks. He and Allison say they were surprised that no one seemed to consider that the coronavirus—though no longer in his system—may have had lasting effects on Buddy’s health.
“If [health officials] had said, ‘Mahoney family, get in the car and come to [a veterinary lab],’ I would have done it,” says Allison, Nobody even mentioned it.”
Cohen, the veterinarian at Bay Street Animal Clinic, said that his team’s focus was on treating Buddy’s symptoms. “We know that we had a very sick patient,” he says, adding that the clinic was only “peripherally involved in the [SARS-CoV-2] case in a lot of ways.”
He says he had three or four conversations with the New York City Health Department and the USDA about Buddy and whether COVID-19 could be related to any of his health problems. “We had zero knowledge or experience with the scientific basis of COVID in dogs,” he says. Even with all the experts on one call, he says, “there was a lot of silence on the phone. I don’t think anybody knew. I really don’t think anybody knew at that point.”
On the morning of July 11, Allison found Buddy in the kitchen throwing up clotted blood. “It looked like it was his insides coming out. He had it all over. It was coming from his nose and mouth. We knew there was nothing that could be done for him from there. What are you going to do for a dog with this? But he had the will to live. He didn’t want to go.”
She and her husband rushed Buddy to the vet, and they made the decision to euthanize him. No one asked Robert about a necropsy, he says—only if he wanted to do cremation or a burial. He chose to have Buddy cremated. Although that day was a blur, he says he knows that if he’d been asked about a necropsy to learn more about the virus in his body, “I would have said, ‘Take whatever you need,’ because I don’t want any other dog to suffer like he did.”
After Buddy’s death, Cohen says he asked the New York City Department of Health whether they needed the dog’s body for any follow-up research. The city had to consult with the USDA and other federal partners, Cohen says they told him. By the time the Department of Health got back to him with the decision to do a necropsy, Buddy had been cremated.
On the day Buddy was euthanized, the vet told Robert that new blood work results indicated that he almost certainly had lymphoma, which could explain many of his symptoms.
The Mahoneys say they’re confident the team at Bay Street did their best for Buddy. They acknowledge that these are uncharted waters for everyone. “I think they are learning as well. It’s all trial and error. And they tried to help us the best way they can,” Allison says, although they still wonder whether COVID played a role in Buddy’s fatal illness.
Cohen says he personally relates to the Mahoneys’ confusion and heartbreak because his father died of COVID-19 two weeks ago in a Florida nursing home at age 94.
“I was unable to see him. And I could say exactly the same criticisms [as the Mahoneys] about how his case was handled—the people didn’t act fast enough,” he says. But like the Mahoneys, he acknowledges that “everyone has good intentions,” grappling with the challenges of treating a horrific, widespread, and little-understood disease.
Knowledge gaps
Buddy’s case highlights an important question: Are animals with underlying conditions more likely to get sick from the coronavirus, just as humans are? It also highlights just how little information is available about infected pets.
Most of what’s known about the coronavirus in companion animals comes from research done on dogs and cats in labs, says Elizabeth Lennon, a veterinarian who specializes in internal medicine at the University of Pennsylvania’s School of Veterinary Medicine, who reviewed Buddy’s medical records for National Geographic. The coronavirus in dogs and cats in the real world could look and act differently than in a lab, and that’s what Lennon’s research is trying to discern.
Despite this being her area of study, Buddy’s vet records were the first she’d seen of an infected pet. While writing a funding proposal to study the virus in dogs and cats recently, she says she realized “this is the first time in my life I've ever written a grant proposal where I’ve cited more press releases and media reports than actual scientific reports.”
Besides the published research on cats and dogs in labs, scientists also have access to the USDA’s public database of every positive animal case in the U.S., with only basic information. The World Organization of Animal Health maintains a similar database of global cases. The Centers for Disease Control and Prevention (CDC) has an extensive toolkit on its website that includes a regularly updated list of known symptoms in animals, but more specific case data is not currently available to the public or the broader research community.
Twelve dogs and at least 10 cats have tested positive in the U.S. Lennon says few case details have been made available to researchers. “What are their signs? How long did they present? What are the blood work changes?” Lennon asks. (Researchers are scrambling to understand which animals the novel coronavirus—which is believed to have originated in bats—can infect.)
Experts involved in these cases will likely publish the details in scientific journals in the next six to 12 months, she says, but while publication of the scientific research on COVID-19 in humans has generally been fast-tracked, “on the vet side of things, we haven’t seen that acceleration yet.”
Buddy’s case also highlights the need to take a more holistic look at all the known cases of infected pets. There has been “no analysis of all cases as a single unit to determine whether there are risk factors other than living in a house with a positive human,” says Shelley Rankin, chief of clinical microbiology at the University of Pennsylvania School of Veterinary Medicine and a colleague of Lennon’s.
It seems that potentially helpful specific case information isn’t always shared among state veterinarians either. State veterinarians typically take the lead when a pet tests positive, and they report details up to the CDC and USDA. Casey Barton-Bahravesh, director of the CDC’s One Health Office in the National Center for Emerging and Zoonotic Infectious Diseases, says she has a weekly call with state veterinarians to share what the CDC is learning about the virus in animals. It’s not clear, however, whether states are learning enough details of each other’s cases. When National Geographic contacted state veterinarians in the seven states where dogs have tested positive, several said that each state is focused on its own cases and communicating directly with the CDC and USDA.
'Cart before the horse'
Lennon says that based on research so far, people can feel fairly confident that healthy dogs and cats don’t pose a big risk of infection to humans or each other in most situations. The primary message from the CDC and the World Organization for Animal Health (OIE) is similar: There is no evidence that animals play a significant role in the spread of the virus. Because of that, they do not recommend widespread testing of pets.
That doesn’t necessarily make sense to Rankin, who says that broader testing of pets would allow public health experts to say with more confidence that pets aren’t being infected on a broad scale (or playing a significant role in the spread off the virus). “We’ve sort of put the cart before the horse,” she says. “If we’re telling the world that prevalence [of animal cases] is low, then we have to look at high numbers."
It’s not clear how many animals in the U.S. have been tested. The CDC’s Barton-Bahravesh says her team is working to collect that data, but it’s difficult because reporting of animal testing is not mandatory.
Lennon says more testing would also shed light on whether animals in certain circumstances—such as those with underlying conditions—are more likely to contract the virus or have the virus for longer.
The second dog to test positive in the U.S., in Georgia, and the sixth dog, in South Carolina, have both died, for example, and their deaths were attributed to other conditions. Similar to Buddy’s case, state veterinarian Boyd Parr says that while there was no compelling evidence that the South Carolina dog’s condition made it more susceptible to the virus, there also wasn’t enough data to say that it didn’t.
“Certainly it is likely the underlying condition could weaken the dog’s natural defenses to a lot of things,” he said in an email.
The CDC’s toolkit includes guidance on caring for and treating a positive pet, and safety guidelines for caregivers, but Lennon says it would be helpful to see guidance that specifies what information veterinarians should collect and what tests they perform on a coronavirus-positive animal to build a consistent and complete picture of how the virus affects pets.
There’s also room to create more opportunities for owners of pets with the virus to connect with researchers. In the Mahoneys’ case, they were keen to have Buddy more closely examined but say that they struggled to connect with experts. “It highlights a missed connection for people who are interested in researching this and owners interested in donating samples," Lennon says.
“My pet was like my son,” Allison Mahoney says. “When he was passing away in front of me, he had blood all over his paws. I cleaned him up before we drove to the vet and stayed with him in the back seat. I said, ‘I will have your voice heard, for all our furry friends. Your voice will be heard, Buddy.’ ”
One of those furry friends is Duke, the Mahoney’s surviving dog. Even though he didn’t get sick, the Mahoneys worry about possible long-term effects of the virus. The puppy has been visibly depressed since Buddy died, the Mahoneys say, and he lies in all of Buddy’s old napping spots.
The Mahoneys hope to pick up Buddy’s ashes this week.
.
www.ncbi.nlm.nih.gov
www.regenstrief.org








www.politico.com
