(Long post... this is Part 1 of 2)
CDC public health news, press releases, government public health news, medical and disease news, story ideas, photos.

www.cdc.gov
Transcript for CDC Telebriefing: CDC Update on Novel Coronavirus
Press Briefing Transcript
Wednesday, February 12, 2020
Please Note: This transcript is not edited and may contain errors.
Operator: Welcome and thank you for standing by. At this time, I would like to inform all participants that your lines have been placed on a listen only mode until the question and answer session of today’s call. Today’s call is also being recorded. If anyone has any objections, you may disconnect at this time. And now I would like to turn the call over to Mr. Benjamin Haynes. Sir, you may begin.
Benjamin Haynes: Thank you Sue. And thank you all for joining us for today’s briefing to update you on CDC’s 2019 novel coronavirus response. We are joined today by Dr. Nancy Messonnier, Director of CDC’s National Center for Immunization and Respiratory Diseases, who will give open remarks before taking your questions. I will now like to turn the call over to Dr. Messonnier.
Dr. Nancy Messonnier: Thank you for joining us. Today, I would like to provide a few updates on important developments over the last few days. First, I want to extend my condolences to the family of the American who died in China over the weekend. As far as we know, this is the first American to die from this new coronavirus. Though more than a thousand people in China have died. My sympathy and my thanks go to the people of China, for those who have lost loved ones and those who are on the front lines battling this virus. In China, they are taking aggressive measures just as we are in the United States. Since we briefed you last, there has been one new confirmed novel coronavirus infection detected in the United States. The new confirmed infection is an individual who returned from Wuhan and was quarantined at Marine Corps Air Station Miramar. This individual was on one of the last Department of State flights out of Wuhan, the epicenter of the outbreak in China. Given the spread of the virus in Wuhan, it is not surprising to see a positive case among people who recently returned from there. That is in fact the reason they are being quarantined. Currently the person has mild illness but is hospitalized. This brings the total number of confirmed positives in the United States to 13. I want to clarify some of the reports that have been circulating about this case. Last Thursday when one of the planes from Wuhan landed at Miramar, a few people were sick and transported to local hospitals for further evaluation. These people were placed in isolation and samples were taken for testing. When running laboratory diagnostics for any disease, anywhere in the world, the ability to match the individual to the specimen is key, and is part of the normal procedures put in place to ensure that that matching is done correctly. But in this situation with this patient, it didn’t work correctly, and the patient was misidentified initially as negative. The issue was identified within 24 hours. The CDC tested the sample, the positive result was conveyed quickly to the local public health and CDC teams. The mishap was unfortunate, but we have corrected this from happening again in the future by adding additional quality control. And it’s really important to emphasize that during this time appropriate infection control precautions were taken around everyone, including around this patient who, again, is doing well. Now I’d also like to update you on our diagnostic test kits. As you know, this is a dynamic, rapidly evolving situation, and our response continues to be based on the latest science. We continue to be flexible to meet the public health challenges that the virus presents, and clearly a success is the CDC rapid development of a diagnostic and rapid deployments to the states, which was clearly important to try to bring the testing closer to patients to avoid delays that have been inherent in sending samples to CDC. When the state receives these test kits, their procedure is to do quality control themselves in their own laboratories. Again, that is part of the normal procedures, but in doing it, some of the states identified some inconclusive laboratory results. We are working closely with them to correct the issues and as we’ve said all along, speed is important, but equally or more important in this situation is making sure that the laboratory results are correct. During a response like this, we know things may not always go as smoothly as we would like. We have multiple levels of quality control to detect issues just like this one. We’re looking into all of these issues to understand what went wrong, and to prevent these same things from happening in the future. Before I take questions, I want to give you a couple more updates. Since the airport screening began in mid-January, CDC and its partners have screened more than 30,000 passengers from China. With the temporary restrictions on travel, we are seeing fewer and fewer travelers from China, especially from Hubei province. Passengers are being funneled through 11 airports, most of these people are coming from parts of mainland China outside of Hubei, show no symptoms and have not been assessed as high risk. Those who passed the screening continue on to their final destination where they self-monitor their health for 14 days in cooperation with their state and local health departments. We’re asking these people to limit their activities and stay home during that 14-day period. Our goal is to be as least restrictive as possible while ensuring the safety and health of all Americans. Since starting our travel restrictions and funneling through airports, we have not detected any cases among returning travelers from China. Most of the U.S. cases were found before the travel restrictions were put in place among travelers who returned from Wuhan and later sought medical care for their illnesses. These cases were picked up by astute clinicians and reported to CDC. We are continually reassessing our recommendations around quarantine and self-monitoring and will continue to work with state and local public health departments to refine and improve this process. Most of the diseases in China, however, we can and should be prepared for this new virus to gain a foothold in the U.S. The goal of the measures we have taken to date are to slow the introduction and impact of this disease in the United States but at some point, we are likely to see community spread in the U.S. Or other countries and this will trigger a change in our response strategy. This will require the effort of all levels of Government, the public health system and our communities as we face these challenges together. We are focusing now on preparing in other areas, including development of guidance for our health care practitioners, and planning for increased demand on our health care system. One important aspect of this is taking steps to make sure there are enough supplies and appropriate guidance to prevent the spread of the disease, especially among health care personnel caring for patients. We understand the importance of providing guidance that health care facilities can implement given the availability of personal protective equipment or PPE supplies. CDC talks regularly with health care industry partners as well as PPE manufacturers and distributors to assess availability of PPE. At this time, some partners are reporting higher than usual demand for select N95 respirators and face masks. CDC does not currently recommend the use of face masks for the general public. This virus is not spreading in the community. If you are sick or a patient under investigation and not hospitalized, CDC recommends wearing a face mask when around other people and before entering a health care provider’s office, but when you are alone, in your home, you do not need to wear a mask. People who are in close contact with someone with novel coronavirus, for example, household contacts and care givers of people with known or suspected 2019, I’m sorry, nCoV 2019, we should wear a face mask if they are in the same room as the patient and that patient is not able to wear a face mask. Health care personnel should wear PPE including respirators when caring for confirmed or possible nCoV patients because they’re in direct contact with those patients which increases their risk of exposure. We will continue to work with our public health partners around the clock to address this public health threat. Some good news this week is that yesterday the first group of 195 people who returned from Wuhan on a State Department flight completed their 14-day quarantine. None of those people have this new virus, and all left March Air Reserve Base successfully and happily returned along the way to their families and their communities. It’s important that people understand that these people being released from quarantine pose no health threat to the surrounding communities or the community that they will be returned to. I want to extend my thanks to them for their cooperation and patience during the quarantine and wish them well as they return to home, work and school. I also want to thank the men and women on March Air Reserve Base and their families for their graciousness while hosting these guests. I also want to say that CDC is working in close collaboration with Japanese health authorities to ensure precautions are being taken to prevent the spread of disease on the Diamond Princess cruise ship as well as making sure the American citizens on that cruise ship are safe. We recognize the continued uncertainty of the current situation. As always CDC public health experts strive to make the best recommendations based on the most up-to-date data. I would be happy to take questions now.
Operator: Thank you. We will now begin the question-and-answer session. In order to provide everyone the opportunity to ask questions, we ask that you limit your questions to one question and one follow up. If you have further questions, simply reinsert yourself back into the queue and your additional questions will be answered as time permits. To ask a question, please press star followed by one. Please ensure your phone is unmuted and record your name clearly when prompted. Again, that is star followed by 1 to ask a question. If you need to withdraw your request press star 2. One moment for the first question. Our first question is from Richard Harris with NPR. You may go ahead.
Richard Harris: Thanks very much. I have a point of clarification and then a question. And my clarification is based on your description of what happened with the test mix up, it sound as though somebody was misidentified as being positive and this person was misidentified as being negative, right, and then you realized that you had the identities wrong and you switched them. I want to make sure that I understand that. Let me ask my question also, which is a little more in-the-weeds, but I’m interested to know what the status is of being able to have a stereological test to identify people who have been exposed but haven’t shown signs of disease. Where is that right now?
Dr. Nancy Messonnier: The answer of the first question is thanks for asking me to clarify because no, that is not exactly right. Because of the problem with identification of the patient, the initial run didn’t include that. You know, as you can imagine, at CDC, there are a large number of specimens being processed, coming in and out, and it’s important that they be identified appropriately so that they’re prioritized. Because of the way that sample was identified, it wasn’t run in that first run. Therefore, it was when the second run was done that we found that it was positive, so it isn’t that somebody else was identified as positive. The sample wasn’t initially run. And the answer to your second question is clearly a stereological test is important in the United States we want to be able to look to see if people zero converted but especially hopefully we’ll be able to help the Chinese look. That test would be really helpful to be able to understand the spectrum of illness that is are there people who are either asymptomatic or mildly symptomatic that have stereological evidence of being exposed to pathogens. We have the beginnings of the stereological tests, because we now have patients in the United States, we’re able to collect additional specimens but we have to collect them over time so that we can have the appropriate timing of specimens to make sure that we understand what the immune response looks like. Once we complete the gathering of those specimens from the patients we’ll be able to pretty rapidly, I would say within a couple of weeks, three weeks, four weeks, be able to have a test available but right now, we’re still in the range of testing of gathering the appropriate specimens from the patients in the U.S. Next question.
Operator: thank you, the next question is from Ivan Couronne with “AFP,” you may go ahead.
Ivan Couronne: Thank you. Have any of the test kits already been actually shipped outside of the U.S.? And if so, which country?
Operator: One moment, please stand by.
Dr. Nancy Messonnier: I’m here. Thank you, I’m sorry. I didn’t get off mute, so excuse me. We have shipped the test kit internationally. I don’t have the specific list of countries in front of me. On last count and this is a couple of days ago, it was somewhere more than 30 countries. It’s important to recognize that this is part of a normal procedure that CDC uses for exactly this kind of reason, to get help make test kits available to other countries who may not have easy access to the same reagents and resources that CDC does, so it’s test kits and each of those countries that are receiving it will go through the same procedures that the recipients in the U.S. are, which is they would do an internal validation verification process before they’d be using those kits, so I also don’t know yet, and we can follow up on this whether any country that has received the kits has gone through that process yet, and whether countries have actually used it. I just don’t have that in front of me. Next question.
Operator: Thank you, the next question is from Hillary Bourke with “Business Insider,” you may go ahead.
Hillary Bourke: Yeah, thanks for taking my call. I had a question about the incubation period. I’m wondering what you think about the new paper that suggests it’s possible the virus might incubate for as long as 24 days in some cases. Have you seen any evidence to support that idea so far?
Dr. Nancy Messonnier: Yeah, so, it’s a really interesting report that has come out. As you can imagine, there is a lot of data coming out and a lot of scientists appropriately are rushing to make sure that any data that they have is in the public realm where all the rest of the scientific community can make use of it. I applaud everyone’s efforts. We have seen in some situations the rush to get data published hasn’t necessarily led to there being the usual level of oversight to make sure that each of the findings is quality controlled, frankly. So, we’re looking at that data closely, but we’re frankly looking at all the other data that’s available that looks at incubation periods. I would say the incubation period is obviously really important for us as we look to make sure that we’re releasing these people safely from quarantine, but the abundance of data, that is available still is consistent with our current stance, which is to use 14 days as the end of that incubation period. I also would say that this is a confusing situation because there may be patients that have mild or even asymptomatic disease that isn’t recognized and when you look at incubation period, you’re starting at the point where a patient is exposed and then counting the days until that patient mounts symptoms. But if there is widespread community spread, for example, it may be that some of those initial exposures aren’t detected and it makes it hard to be sure about the actual incubation period. Our CDC staff there actually are something like 50 separate modeling groups in the United States that are working with us on exactly these issues. It’s important that we work with all of these modelers because they have different symptoms than we do, but we’re working with all of the greatest minds in the country and globally try to pin down these facts as much as we can, and we still think that for today, for now, 14 days is the right interval to use. Next question.



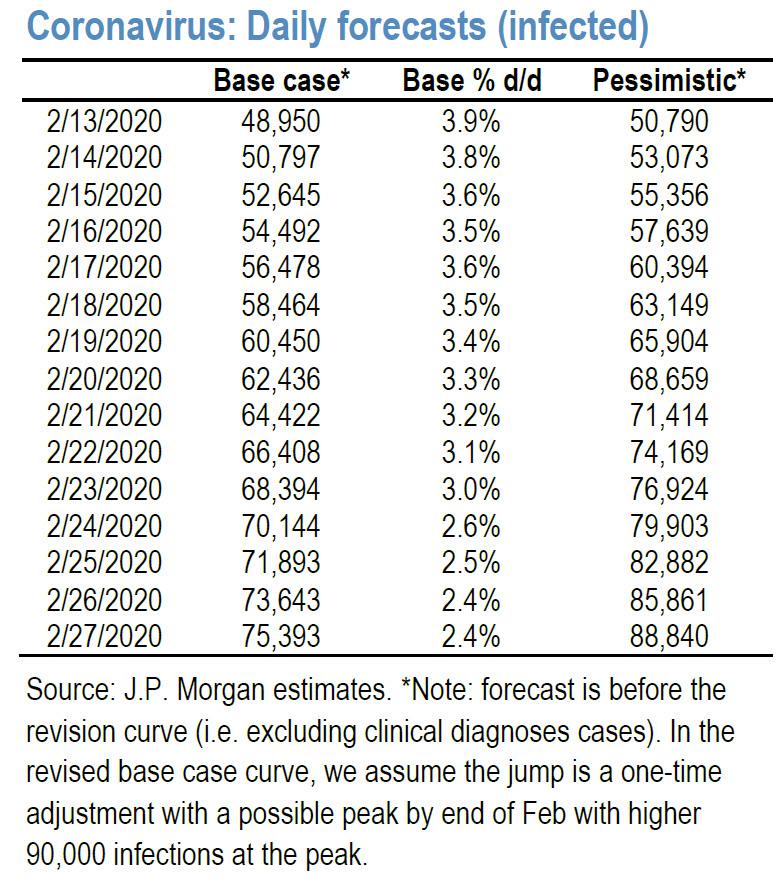
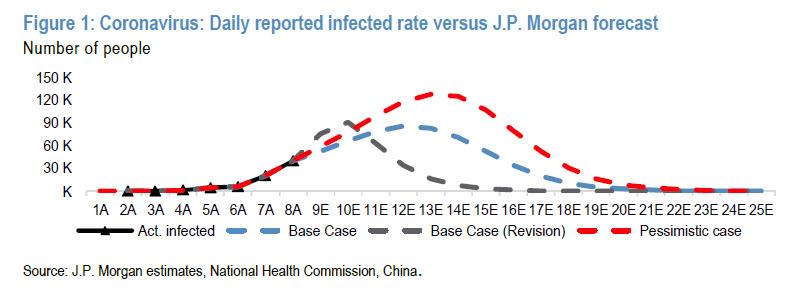
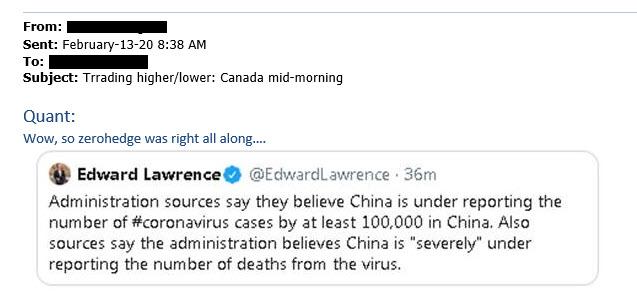
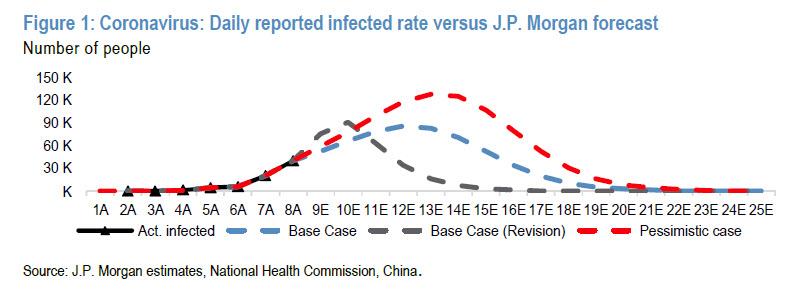
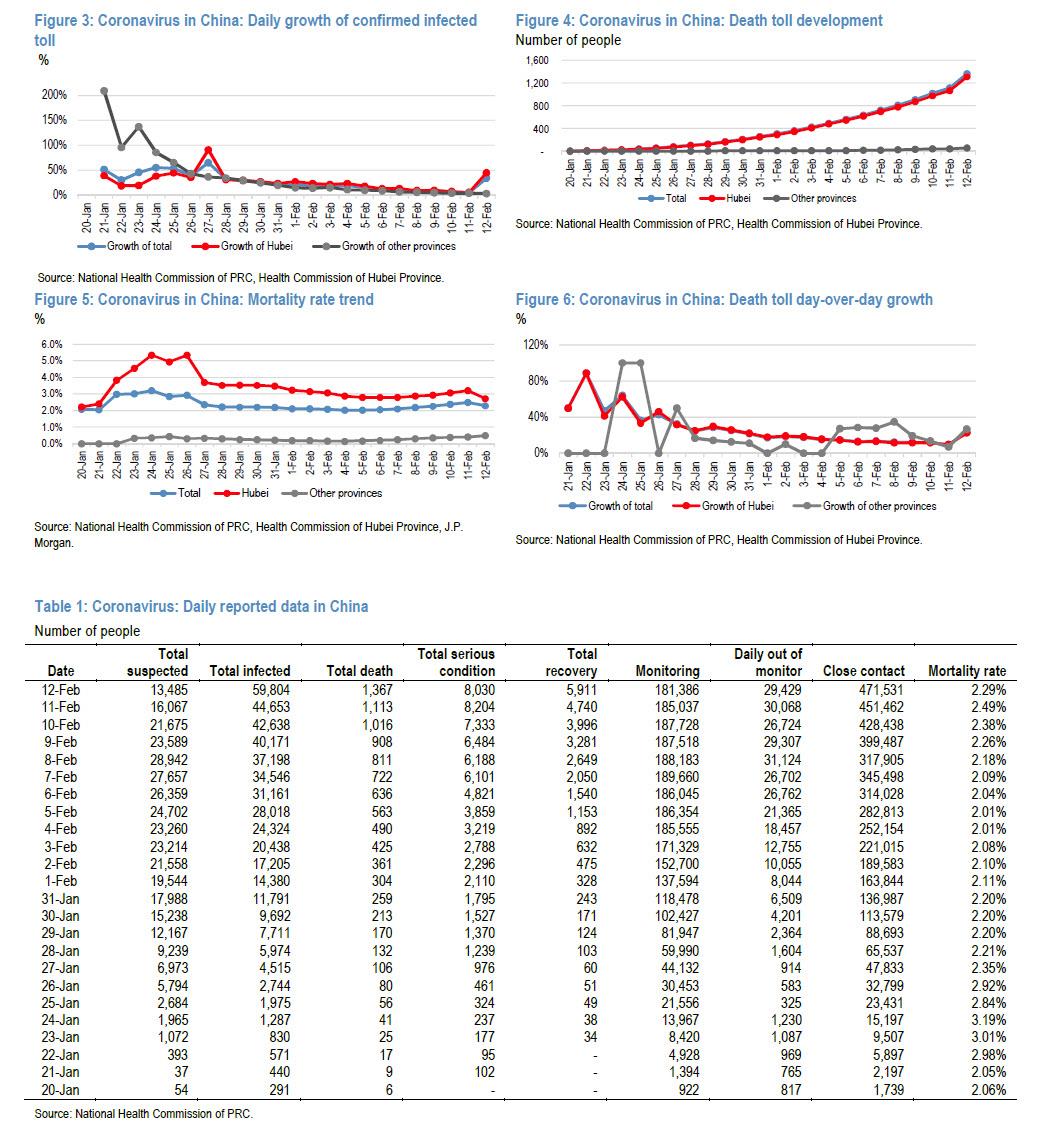



 But it is confirmation to all of us who have been watching this for almost a month that we did get it right, and we were not doomers running around with our head on fire for the thrill of the doom.
But it is confirmation to all of us who have been watching this for almost a month that we did get it right, and we were not doomers running around with our head on fire for the thrill of the doom.